In what seems like the blink of an eye, all of the data inputs feeding the connected health ecosystem are wirelessly enabled and pretty easy to set up. It is this realization that stimulated me and my coauthors to write The Internet of Healthy Things.
But it wasn’t always that way.
Just a few years back, we toiled to get information out of what were then ‘dumb’ sensors – blood pressure cuffs, weight scales, glucometers and the like. Both the engineering required and the patient involvement needed to make these early systems work were burdensome. The first phase of this journey was enabled by now nearly-obsolete home hub devices which typically used analog phone line connections and modem technology. The patient had to connect wires to set it up and then push a button to upload any data, hoping the transmission would go through. Sometimes the patient thought she was transmitting when, in fact, no data was flowing. Often, connections would work one day and break the next.
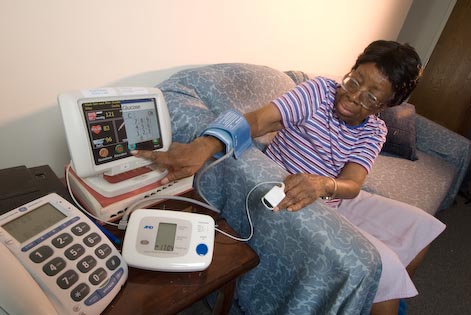
In order to minimize patient frustration and all of the effort required, we asked our patients to ‘batch upload’ readings once a week or so. They would capture whatever data we asked for (blood pressures, glucose readings, etc.) as prescribed, but only upload that data periodically. When it worked, this system actually worked well. We studied this program and made several observations that became guiding principles for designing future interventions.

One key principle that we have applied several times is the understanding that these tools allow for a very fine measurement of patient engagement. Patients who participated in these early programs and put up with of the cumbersome set up — button pushing, uploading, etc. — were a bit like the earliest settlers moving across the US in the 1800s. These patient pioneers cared enough about their disease to make all of this extra effort in order to share their health data with their doctor. When we looked at the correlation between frequency of upload and clinical outcomes, we found a positive relationship for both diabetes and hypertension. The more engaged patients were, as measured by uploads, the better their clinical outcomes. In retrospect, our sample was probably enriched not for tech savvy users (doctors prescribed these tools based on disease severity) but for those who were motivated to improve their health.
We also learned that provider engagement mattered. For a given sample, the more a nurse, diabetic educator or other front-line clinician logged in to the clinician portal, the better the outcomes of the group.
Another important, early finding was that patients dropped out of the program or gave up for a couple of reasons. One was difficulty in using the technology. This became glaringly obvious once we had passive data collection devices in the field. With passive data collection, the patient took their blood pressure as they normally would and the data flowed from device to hub to Internet with no extra work on the patient’s part. Set up for these systems was much easier too – no phone lines to mess with. We were, for the most part, able to achieve what is known in the industry as ‘plug and play.’

When we compared these passive data upload systems with the aforementioned push-button systems, we found patients uploaded 3X more often with the passive systems. The tricky set up and the pushing of a button was too much to ask for many of our chronically ill patients. These observations led to a design battle cry for ‘wear and forget’ sensors, passive data upload and frictionless technology (e.g., no set up).
The second reason we found patients dropped out was if they perceived that their doctor was not paying attention to their data. You can see the logic – my doctor recommended this to me, it is a lot of extra work and if she is not acknowledging that work, I’m going to drop out. This logic ignores the notion that we should be intrinsically motivated to improve our own health, but we’ll leave that for a future post.
The flip side of this phenomenon is that when patients perceive the doctor cares about their data, they try even harder to meet their health goals. This led to our employing the design principle of the sentinel effect (we behave differently when we know we’re being watched, especially by someone whose opinion we care about).

So, what’s the paradox? As the Internet of Things has become a reality, increasingly sensors are designed to easily offload their data to the cloud. Set up is easy, always through your smartphone, connections are much more robust and data flows effortlessly. Wear and forget is becoming a reality and new products from companies like Proteus Digital Health and MC 10 take disposable/wearable/ingestible to a new level. But as we perfect systems to capture health data and make it easy, people tend to forget about the data feedback loops that allow for improvements in health.
Yes, we’ve done a great job of frictionless data capture, but we’ve lagged on engagement. Designers of consumer mobile apps are constantly studying how to employ mobile technology to keep users engaged with their content. News apps get your attention through banners, notifications, etc. when there is fresh content. But I can’t think of a health app that does a good job at this. For example, my favorite activity tracker app sends me the same three messages every day, “You’re almost there,” “You reached your goal” and “You’ve outdone yourself.” It’s no wonder that the new industry phrase for measuring device success is “time to drawer.” Or, stated another way, how long did you wear the thing before you got bored with it and threw it in the drawer?
So, the paradox results from two observable facts. First, because it was such an engineering challenge to get data flowing in a frictionless manner, most of the current devices and systems were designed by engineers (quantitative people) and adopted early by other quantitative people (e.g., quantified selfers). Early adopters were engaged by their own data and probably needed less in the way of software engagement. Second, creating sustained engagement via software is hard, especially in health-related interventions. The most engaging apps are still in the communication/social realm – WeChat, SnapChat, Instagram, etc. They harness the natural human need to share and interact with others. Who wants to be reminded they are overweight? Or have high blood pressure? Or have to stick their finger twice a day to check their blood sugar? The engagement challenge here is orders of magnitude more difficult.

Achieving passive data upload (we’re not 100% done but the end is in sight) is a feat we can all be proud of. If we’re going to make connected health a widespread reality in the lives of consumers and patients, we have to double down on engagement. We need to bring together first class designers, motivational psychologists, marketing scientists, behavioral economists and all others who understand how to build sticky apps and services. We owe it to our patients to create well-designed, engaging apps. If we don’t, they’ll be paying attention to Instagram and our connected health devices will lie fallow in a corner somewhere.
We’re building such a team at Partners Connected Health and I find their early work inspiring.
Wanna share this post
- Click to share on Twitter (Opens in new window)
- Click to share on Facebook (Opens in new window)
- Click to share on LinkedIn (Opens in new window)
- Click to share on Tumblr (Opens in new window)
- Click to share on Pocket (Opens in new window)
- Click to share on Reddit (Opens in new window)
- Click to share on Pinterest (Opens in new window)
- Click to share on WhatsApp (Opens in new window)
- Click to share on Telegram (Opens in new window)
- Click to share on Skype (Opens in new window)
